Helen Wolkowicz is a Montreal-based writer and herself the mother of a micro-preemie who received care at the Royal Victoria Hospital’s NICU 14 years ago. She has been helping raise funds for the unit for the last five years.
Montreal — Tucked away at the Royal Victoria Hospital is a unit that is rarely mentioned. Expectant moms and dads are whisked through it as part of prenatal tours but they do not linger, because no one likes to talk about this place. The Neonatal Intensive Care Unit houses critically ill newborns and premature babies, and every year it saves hundreds of them.
Olivia Kerub is one of those babies. She was born last November after spending a mere 23 weeks in the womb, and weighed 480 grams, or just over one pound — one of the smallest newborns the unit has cared for in recent years.

A pregnancy is deemed full-term at 39 weeks’ gestation; babies born before 37 weeks are considered premature. An extremely low-birth-weight infant, or micro-preemie, weighs less than 1,000 grams and is born before 28 completed weeks of gestation. Such babies have immature lungs, hearts, kidneys, gastrointestinal tracts and so forth. They require intensive support and are at great risk of disability or death.
Olivia’s parents, Montrealers Valérie Daude Carrière and Philip Kerub, had been trying to conceive a child for years without success, despite the fact that Carrière was only in her 20s. They had been living outside Canada for a few years, and decided to undergo in vitro fertilization last summer in Miami, where they insisted on implanting two embryos to maximize the chances of pregnancy.
It worked. Carrière, at 24, became pregnant with twins — a boy and a girl.
She let herself indulge in idyllic dreams of what her pregnancy would be like.
“I was making all kinds of plans that had piled up over the years,” she said. “I dreamed of shopping for baby things with my big belly. The nightmare was finally over.”
In fact, it was just beginning.
When Carrière was almost halfway through a full-term pregnancy, just shy of 20 weeks’ gestation, she was jolted awake at 5 a.m. by violent cramps. Her husband rushed her from their downtown home to the Royal Victoria Hospital, where doctors discovered that one of the babies, the boy, was already crowning.
“ ‘I think your wife is having a miscarriage,’ ” Kerub remembers being told by the resident. “It was the worst shock of my life, like I was just hit by lightning.”
If a baby is born before 24 weeks’ gestation, there is a slim chance of survival.
Doctors administered magnesium sulphate to diminish uterine contractions. Carrière was confined to a hospital bed, with her legs raised higher than her shoulders to keep the babies safely in place.
The next days were fraught with complications. Carrière winced and cried in her sleep from the pain of contractions.
Around the 22-week mark, the situation became critical. Carrière had an E. coli infection and high fever. One of the babies’ umbilical cords emerged from the uterus, a rare and dangerous situation. The boy’s amniotic sac — which provides a sterile environment safe from infection — ruptured. He began descending into the pelvis, which exerted pressure on the umbilical cord, decreasing blood supply and oxygen. Without the amniotic sac, he was exposed to vaginal bacteria.
Hour by hour, the status of both babies fluctuated. Heartbeat. No heartbeat.
“It got to the point where the good news was hurting me as much as the bad news. I had no more emotion to be happy,” said Kerub. “Despair is easier to fall into than hope. The hopes you just had about their survival get crushed and you die inside. Despair is easier because you get it over with. It’s done.” Carrière held on for her twins. She held on for her life.

Dr. Guilherme Mendes Sant’Anna, associate professor of pediatrics at the McGill University Health Centre, and neonatologist at the Royal Victoria Hospital’s NICU, was part of Carrière’s medical team.
“At about 22 weeks, we discussed the chances for the baby boy,” he recounted. “Half of the body was inside the uterine cavity and half of his body was outside, making him very vulnerable.”
Concerned for the mother’s life, the team of doctors discussed terminating the pregnancy.
“There’s always a balance between inducing delivery to focus on the mother’s health or continuing with the pregnancy to try to gain some time and increase the chances of the baby becoming viable,” Sant’Anna said. “It’s a very difficult choice.”
What happened next was something Sant’Anna had never encountered in his 23 years as a neonatologist: “The baby boy stayed in a dangerously low position for several days and protected his sister from dropping out of the uterus herself. The girl was fine, resting comfortably in her membrane.”
But Carrière was not fine. She contracted another E. coli infection. Her blood pressure shot up. Her heartrate skyrocketed to 180. Her temperature spiked.
Paralyzed by fear, Kerub could only watch as his wife’s eyes rolled to the back of her head; her body shook uncontrollably; her face was ashen. She was septic.
All three lives were in peril, and the birthing process was now inevitable.
The tiny boy was born. He did not survive.
“They took him to a warming table. Then, the light closed on the table,” Carrière recounted, choking back tears. “A nurse brought him to me and asked, ‘Would you like to hold him?’ It just clicked. It was time to say goodbye.”
After she give birth, Carrière’s condition stabilized briefly. The other baby remained secure in the womb. But there would be no reprieve, no time to grieve the loss of her son.
Less than eight hours later, Carrière began having fierce contractions again. An ultrasound revealed the baby was in a breech position. Because of the trauma the mother had just endured, a caesarean section was not an option.
“My stomach was turning. I couldn’t breathe. I prayed for a miracle,” Kerub recalled.
The baby girl was delivered feet first, still in her amniotic sac, which provided vital defence against infection. Olivia was immediately taken to the NICU, where the fight for her life continued.

For the uninitiated, seeing a micro-preemie can evoke conflicting emotions
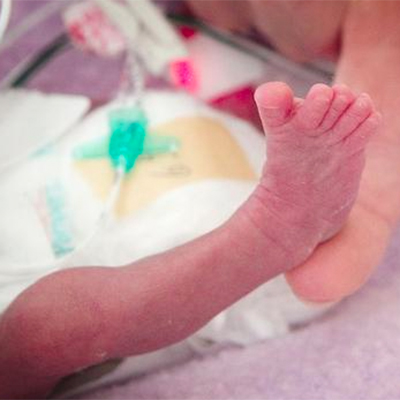
of joy and sorrow. Physically, they are the antithesis of the Gerber baby. Their paper-thin skin is translucent and has a purplish-brownish hue due to lack of body fat, which makes their veins and arteries visible. Since this top layer of skin is still undeveloped, parents must refrain from caressing their baby’s skin as this will inflict pain.
Carrière remembers her reaction when meeting her daughter for the first time: “I looked at her and I was speechless. She was so tiny. Her little foot was no bigger than my pinky and it was kicking. It was as though she was trying to let me know that she was alive.”
The next 48 hours were critical. Olivia was put on a ventilator, a central line was inserted to deliver fluids and nutrition, and she was hooked up to a monitor to measure her vital signs. A multidisciplinary team including neonatologists, nurses, nurse practitioners, pharmacists, respiratory therapists and technicians was working in overdrive
The first days of life are gruelling for extremely immature infants, Sant’Anna explained. As for the parents, they’re overwhelmed and retain little information.
In Olivia’s case, their primordial question was: “Does she have a chance?” to which Sant’Anna responded: “Yes.”
“I try to avoid giving numbers,” he explained. “Many variables can affect the baby’s survival. It becomes clearer day by day — if you experience complications or if you don’t. It’s very individual. That’s how neonatology should be.”
Olivia’s size invoked special medical protocols: minimal handling of the infant to protect her fragile skin and keep essential humidity in the isolette; a new practice for bathing to mitigate the risk of sepsis using a wipe imbued with the antiseptic chlorhexidine; privacy screens to quarantine her. Nobody could touch her other than her parents, and the nurse and doctor on duty.
“These babies are very fragile. The less interventions you do, the better it is for the baby. We tried to mimic the womb’s conditions,” Sant’Anna said. “The first week of life is very critical — it’s a transitional phase to life outside the mother.”

It’s a roller-coaster ride for preemies in the NICU. And the baby’s well-being is inextricable from the parents’ emotional state. Just as the baby appears to be making steady progress, an unexpected setback can suddenly arise; parents who had found brief stability find themselves plunged into anguish.
NICU nurse Marnie Chuipka, who met baby Olivia shortly after her birth, said the reverse is also true: “Whatever you’re feeling, the baby will pick up on it.”
As stressful and daunting as the NICU can be, lighting and noise levels are kept as low as possible in the hopes of providing a soothing environment for preemies and sick infants.
But the hush is often pierced by the sudden beeping and alerts of monitors, which can send stress levels soaring for anxious parents. It can be hard for parents not to become obsessed with the monitor that displays their infant’s vital signs. Carrière remembers that her fear of what she would find when visiting her daughter was so intense, she couldn’t enter the unit without her husband by her side, because she was worried about fainting.

During those anxious first days, NICU nurses provide much-needed support.
It is common practice to assign a primary nurse to neonates who face a lengthy hospital stay. This fosters a symbiosis between the baby and the nurse. Babies benefit from having a nurse who understands their personalities and quirks. Parents appreciate the consistency of interacting with the same person and feel reassured when they cannot be physically present. For the nurse, the reward is seeing the preemie not only survive, but thrive.
“We do family-centred care. Yes, we take care of the baby, but the family as well,” says Chuipka. “There are very stressful situations in the NICU. You build a relationship with the parents so that they trust you and so that they’re able to go home and sleep.”
Chuipka says the toughest part of her job is seeing parents suffer on especially strenuous days.
“Parents have dreams and make plans for their unborn babies. They don’t make plans for this. They dream about going home and decorating the room. Sometimes it ends with no baby — to see them leave alone is heartbreaking.”
Sitting in the NICU day after day can take its toll on parents. It is agonizing to be unable to protect and cradle your baby, especially when medical complications arise. Parents often feel helpless.
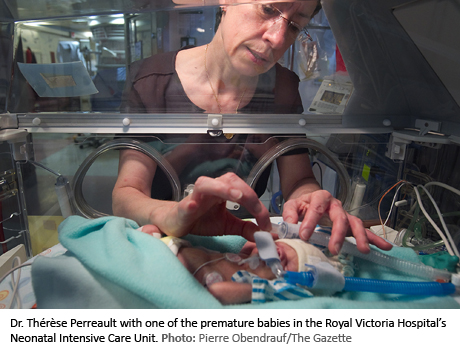
Dr. Thérèse Perreault oversees the NICUs of both the Royal Victoria and the Montreal Children’s Hospital.
“There is always hope in the NICU,” she said.
Despite their tiny size, preemies have formidable resilience and their fight for life is fierce — this is the beautiful and complex dichotomy of the extremely premature infant.
“We have cautious expectations about their outcomes, yet when they come back to visit us, they constantly surprise us by how well they do,” said Perreault, who is an associate professor of pediatrics at the McGill University Health Centre and director of the MUHC’s Division of Neonatology. “Because of the brain’s plasticity, preemies have a great capacity to compensate, adapt and overcome many hurdles. This is why there is always hope.”
Chuipka sees this on a regular basis. “They’re so tiny and look so weak, but they are so strong — so resilient.”
On Day 5 of Olivia’s life, her parents were finally permitted to touch their child — but only her toe. “When I pushed, she pushed back,” Carrière said. “She was full of life.”
After 26 days, another euphoric event. The mother was able to hold her newborn. For preemies, kangaroo care is recommended; it consists of holding the diapered, undressed infant in an upright position on a parent’s bare chest. The baby’s head is turned so that the ear is above the parent’s heart. Kangaroo care helps regulate the baby’s body temperature, heart rate and breathing. It is also believed to contribute to weight gain.
Carrière was told she could hold her baby for 30 minutes only. Once Olivia was in position against her mother’s chest, her father’s eyes were glued to the monitor, scrutinizing the vital signs. Olivia’s vitals were so steady, a full hour of kangaroo care was permitted.
Against the odds, and to the surprise of the medical personnel, Olivia sailed through her 142-day stay in the NICU without any serious medical complications. She was discharged at the robust weight of 3,500 grams, or about 7 pounds, 7 ounces. The cost for such a lengthy stay? Perreault said it’s about $10,000 per day, covered by the Régie de l’assurance maladie du Québec.
Last year, the Royal Victoria Hospital’s NICU cared for 350 babies, while the Montreal Children’s Hospital’s NICU had 410 admissions. In 2015, these two NICUs will merge and move to the Glen campus in the new McGill University Health Centre superhospital in N.D.G.

Today, at 9 months old, Olivia is developing beautifully, with chubby cheeks and inquisitive eyes.
She no longer requires oxygen during the day and is expected not to need it at night in the near future.
For the next five years, she will be in a program for extremely low-birth-weight babies and will be monitored at the Montreal Children’s Neonatal Follow-Up Clinic to ensure she reaches her developmental and growth milestones.
Carrière said she and Kerub credit the extraordinary care and devoted staff at the NICU for their tiny survivor.
“If you want miracles — this is where it happens.”
© Copyright (c) The Montreal Gazette

MONTREAL — As of April 2015, the Royal Victoria Hospital’s NICU will move to the McGill University Health Centre’s new Glen site, merging with the Montreal Children Hospital’s NICU. Among the features of the new unit:
- Each baby will have a private room.
- If necessary, surgery could be performed in the baby’s room.
- Mothers will be able to pump breast milk in their baby’s room.
- Music therapy will be offered.
- Bigger windows will allow for more natural light.
© Copyright (c) The Montreal Gazette

MONTREAL — There are five hospitals in Montreal equipped with Level 3 Neonatal Intensive Care Units:
- Centre hospitalier Ste-Justine
- Hôpital Maisonneuve-Rosemont
- Jewish General Hospital
- Montreal Children’s Hospital
- Royal Victoria Hospital.
A Level 3 NICU has an array of staff and specialized equipment to care for the smallest and sickest newborns 24/7.
According to the Canadian Premature Babies Foundation, one in 10 babies in Canada is born prematurely.

